Vitamin K Deficiency: Signs, Causes, and Prevention Guide
“`html
Understanding Vitamin K Deficiency: Causes, Symptoms, and Solutions
Vitamin K is an essential nutrient that plays a critical role in blood clotting and bone metabolism. While it is less discussed than vitamins D or B12, a deficiency can lead to serious health complications. Unlike fat-soluble vitamins, the body stores only small amounts of vitamin K, making consistent dietary intake or supplementation necessary. This article explores the nuances of vitamin K deficiency, from its underlying causes to practical prevention strategies.
What Is Vitamin K and Why Does It Matter?
Vitamin K exists in two primary forms: K1 (phylloquinone) and K2 (menaquinone). Vitamin K1 is primarily found in green leafy vegetables like spinach and kale, while K2 is present in fermented foods, certain meats, and even produced by gut bacteria. Both forms are vital for activating proteins that regulate blood coagulation and calcium metabolism in bones and arteries.
Without adequate vitamin K, the body struggles to form clots, increasing the risk of excessive bleeding. In severe cases, this can become life-threatening. Additionally, low vitamin K levels have been linked to weakened bones and a higher likelihood of arterial calcification, which can contribute to cardiovascular disease. Given these risks, recognizing the signs of deficiency early is crucial for maintaining long-term health.
Common Causes of Vitamin K Deficiency
The most frequent causes of vitamin K deficiency fall into three broad categories: dietary insufficiency, malabsorption issues, and medication interactions. Understanding these triggers can help individuals take proactive steps to mitigate their risk.
Dietary insufficiency is the most straightforward cause. Many people do not consume enough vitamin K-rich foods, particularly if their diets lack green vegetables, fermented products, or animal-based foods. Certain populations—such as older adults, individuals with eating disorders, or those following restrictive diets—are particularly vulnerable.
Malabsorption problems also play a significant role. Conditions like celiac disease, Crohn’s disease, or bile duct obstructions can impair the body’s ability to absorb fat-soluble vitamins, including vitamin K. Additionally, prolonged use of antibiotics can disrupt gut bacteria that naturally produce K2, further depleting stores.
Medications can interfere with vitamin K in unexpected ways. Blood thinners like warfarin are designed to counteract vitamin K’s clotting effects, requiring careful dietary management to maintain balance. Conversely, other drugs, such as certain anticonvulsants or cholesterol-lowering medications, may reduce vitamin K absorption or increase its breakdown in the body.
Spotting the Signs: Symptoms of a Deficiency
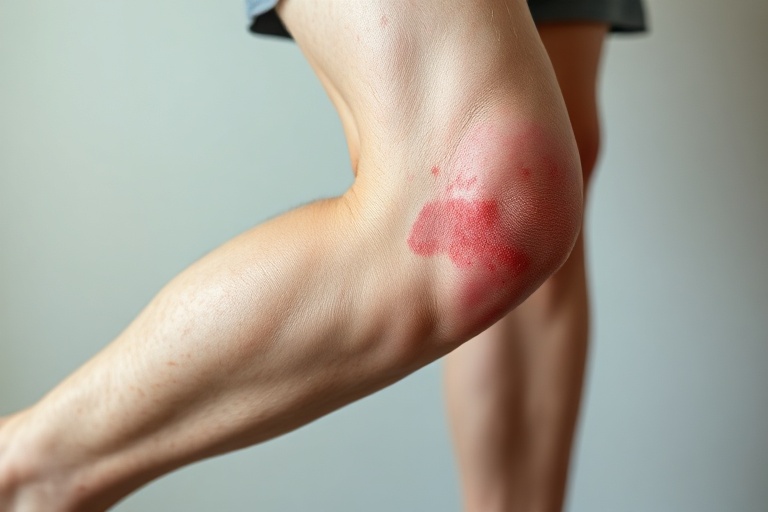
Vitamin K deficiency often presents subtly at first, with symptoms that can be mistaken for other conditions. One of the earliest indicators is easy bruising or prolonged bleeding from minor cuts or injuries. Women may notice heavier menstrual bleeding than usual, while others might experience frequent nosebleeds or bleeding gums, particularly after brushing.
In infants, vitamin K deficiency can be especially dangerous. Newborns are born with low vitamin K levels, and without a prophylactic injection at birth, they are at risk of a rare but severe condition called hemorrhagic disease of the newborn. Symptoms include unexplained bleeding, including in the brain, which can lead to neurological complications if untreated.
Chronic deficiency over time may also manifest in less obvious ways. Some individuals report persistent fatigue or weakness, while others develop unusual calcium deposits in their arteries or bones, leading to stiffness or joint pain. If left unaddressed, these long-term effects can significantly impact quality of life.
Prevention and Treatment: How to Maintain Healthy Vitamin K Levels
Preventing vitamin K deficiency starts with a balanced diet rich in the right foods. Leafy greens—such as spinach, Swiss chard, and Brussels sprouts—are excellent sources of K1. For K2, fermented foods like natto, sauerkraut, and certain cheeses can be particularly effective. Including these in meals regularly can help maintain adequate levels without relying solely on supplements.
For individuals at higher risk—such as those with malabsorption disorders or on blood thinners—supplementation may be necessary. However, it’s important to consult a healthcare provider before starting any new supplement regimen, especially if taking medications like warfarin. In some cases, adjusting medication doses or monitoring vitamin K intake more closely may be required to avoid complications.
Regular health check-ups can also help detect deficiencies early. Blood tests measuring prothrombin time (PT) or international normalized ratio (INR) can indicate whether clotting function is impaired. For those with chronic conditions, working with a dietitian to tailor a vitamin K-friendly meal plan can be a practical step toward prevention.
In cases where deficiency has already developed, treatment typically involves targeted supplementation under medical supervision. Intravenous or oral vitamin K doses can quickly restore levels, particularly in emergency situations involving uncontrolled bleeding. However, the underlying cause—whether dietary, absorption-related, or medication-induced—must also be addressed to prevent recurrence.
Who Is Most at Risk?
Certain groups face a higher likelihood of developing vitamin K deficiency due to biological, lifestyle, or medical factors. Infants, as previously mentioned, are particularly vulnerable without proper intervention. Older adults may also be at risk due to reduced dietary intake, decreased gut bacteria production of K2, or medications that interfere with absorption.
Individuals with chronic gastrointestinal disorders—such as inflammatory bowel disease (IBD) or liver disease—often struggle with malabsorption. Additionally, those who have undergone bariatric surgery may find it challenging to absorb fat-soluble vitamins, including vitamin K. People with eating disorders or alcohol dependence may also have insufficient dietary intake or impaired absorption.
Monitoring vitamin K status is especially important for these populations. For example, health-conscious readers looking to optimize their nutrition may benefit from tracking their intake of vitamin K-rich foods and discussing supplementation with a healthcare provider.
Conclusion: Taking Control of Your Vitamin K Intake
Vitamin K deficiency is a silent but potentially serious condition that can have far-reaching consequences. From excessive bleeding to weakened bones and cardiovascular risks, the stakes are high enough to warrant attention. The good news is that awareness and proactive measures—such as diversifying your diet, addressing underlying health issues, and seeking professional guidance—can significantly reduce the risk.
For those already managing chronic conditions or taking medications that affect vitamin K, regular monitoring and adjustments are key. By staying informed and making intentional choices about nutrition and healthcare, individuals can safeguard their well-being and avoid the pitfalls of deficiency. Whether through dietary changes, supplementation, or medical intervention, taking control of vitamin K levels is a small but meaningful step toward long-term health.